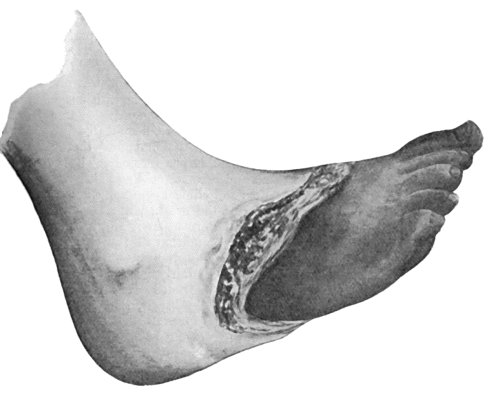
Fig. 20.—Senile Gangrene of the Foot, showing line of demarcation.
While the varieties of gangrene included in this group depend primarily on interference with the circulation, it is to be borne in mind that the clinical course of the affection may be profoundly influenced by superadded infection with micro-organisms. Although the bacteria do not play the most important part in producing tissue necrosis, their subsequent introduction is an accident of such importance that it may change the whole aspect of affairs and convert a dry form of gangrene into one of the moist type. Moreover, the low state of vitality of the tissues, and the extreme difficulty of securing and maintaining asepsis, make it a sequel of great frequency.
Senile Gangrene.—Senile gangrene is the commonest example of local death produced by a gradual diminution in the quantity of blood passing through the parts, as a result of arterio-sclerosis or other chronic disease of the arteries leading to diminution of their calibre. It is the most characteristic example of the dry type of gangrene. As the term indicates, it occurs in old persons, but the patient's age is to be reckoned by the condition of his arteries rather than by the number of his years. Thus the vessels of a comparatively young man who has suffered from syphilis and been addicted to alcohol are more liable to atheromatous degeneration leading to this form of gangrene than are those of a much older man who has lived a regular and abstemious life. This form of gangrene is much more common in men than in women. While it usually attacks only one foot, it is not uncommon for the other foot to be affected after an interval, and in some cases it is bilateral from the outset. It must clearly be understood that any form of gangrene may occur in old persons, the term senile being here restricted to that variety which results from arterio-sclerosis.
Clinical Features.—The commonest seat of the disease is in the toes, especially the great toe, whence it spreads up the foot to the heel, or even to the leg (Fig. 20). There is often a history of some slight injury preceding its onset. The vitality of the tissues is so low that the balance between life and death may be turned by the most trivial injury, such as a cut while paring a toe-nail or a corn, a blister caused by an ill-fitting shoe or the contact of a hot-bottle. In some cases the actual gangrene is determined by thrombosis of the popliteal or tibial arteries, which are already narrowed by obliterating endarteritis.
It is common to find that the patient has been troubled for a long time before the onset of definite signs of gangrene, with cold feet, with tingling and loss of feeling, or a peculiar sensation as if walking on cotton wool.
The first evidence of the death of the part varies in different cases. Sometimes a dark-blue spot appears on the medial side of the great toe and gradually increases in size; or a blister containing blood-stained fluid may form. Streaks or patches of dark-blue mottling appear higher up on the foot or leg. In other cases a small sore surrounded by a congested areola forms in relation to the nail and refuses to heal. Such sores on the toes of old persons are always to be looked upon with suspicion and treated with the greatest care; and the urine should be examined for sugar. There is often severe, deep-seated pain of a neuralgic character, with cramps in the limb, and these may persist long after a line of demarcation has formed. The dying part loses sensibility to touch and becomes cold and shrivelled.
All the physical appearances and clinical symptoms associated with dry gangrene supervene, and the dead portion is delimited by a line of demarcation. If this forms slowly and irregularly it indicates a very unsatisfactory condition of the circulation; while, if it forms quickly and decidedly, the presumption is that the circulation in the parts above is fairly good. The separation of the dead part is always attended with the risk of infection taking place, and should this occur, the temperature rises and other evidences of toxæmia appear.
Prophylaxis.—The toes and feet of old people, the condition of whose circulation predisposes them to gangrene, should be protected from slight injuries such as may be received while paring nails, cutting corns, or wearing ill-fitting boots. The patient should also be warned of the risk of exposure to cold, the use of hot-bottles, and of placing the feet near a fire. Attempts have been made to improve the peripheral circulation by establishing an anastomosis between the main artery of a limb and its companion vein, so that arterial blood may reach the peripheral capillaries—reversal of the circulation—but the clinical results have proved disappointing. (See Op. Surg., p. 29.)
Treatment.—When there is evidence that gangrene has occurred, the first indication is to prevent infection by purifying the part, and after careful drying to wrap it in a thick layer of absorbent and antiseptic wool, retained in place by a loosely applied bandage. A slight degree of elevation of the limb is an advantage, but it must not be sufficient to diminish the amount of blood entering the part. Hot-bottles are to be used with the utmost caution. As absolute dryness is essential, ointments or other greasy dressings are to be avoided, as they tend to prevent evaporation from the skin. Opium should be given freely to alleviate pain. Stimulation is to be avoided, and the patient should be carefully dieted.
When the gangrene is limited to the toes in old and feeble patients, some surgeons advocate the expectant method of treatment, waiting for a line of demarcation to form and allowing the dead part to be separated. This takes place so slowly, however, that it necessitates the patient being laid up for many weeks, or even months; and we agree with the majority in advising early amputation.
In this connection it is worthy of note that there are certain points at which gangrene naturally tends to become arrested—namely, at the highly vascular areas in the neighbourhood of joints. Thus gangrene of the great toe often stops when it reaches the metatarso-phalangeal joint; or if it trespasses this limit it may be arrested either at the tarso-metatarsal or at the ankle joint. If these be passed, it usually spreads up the leg to just below the knee before signs of arrestment appear. Further, it is seen from pathological specimens that the spread is greater on the dorsal than on the plantar aspect, and that the death of skin and subcutaneous tissues extends higher than that of bone and muscle.
These facts furnish us with indications as to the seat and method of amputation. Experience has proved that in senile gangrene of the lower extremity the most reliable and satisfactory results are obtained by amputating in the region of the knee, care being taken to perform the operation so as to leave the prepatellar anastomosis intact by retaining the patella in the anterior flap. The most satisfactory operation in these cases is Gritti's supra-condylar amputation. Hæmorrhage is easily controlled by digital pressure, and the use of a tourniquet should be dispensed with, as the constriction of the limb is liable to interfere with the vitality of the flaps.
When the tibial vessels can be felt pulsating at the ankle it may be justifiable, if the patient urgently desires it, to amputate lower than the knee; but there is considerable risk of gangrene recurring in the stump and necessitating a second operation.
That amputation for senile gangrene performed between the ankle and the knee seldom succeeds, is explained by the fact that the vascular obstruction is usually in the upper part of the posterior tibial artery, and the operation is therefore performed through tissues with an inadequate blood supply. It is not uncommon, indeed, on amputating above the knee, to find even the popliteal artery plugged by a clot. This should be removed at the amputation by squeezing the vessel from above downward by a “milking” movement, or by “catheterising the artery” with the aid of a cannula with a terminal aperture.
It is to be borne in mind that the object of amputation in these cases is merely to remove the gangrenous part, and so relieve the patient of the discomfort and the risks from infection which its presence involves. While it is true that in many of these patients the operation is borne remarkably well, it must be borne in mind that those who suffer from senile gangrene are of necessity bad lives, and a guarded opinion should be expressed as to the prospects of survival. The possibility of the disease developing in the other limb has already been referred to.
Embolic Gangrene (Fig. 21).—This is the most typical form of gangrene resulting from the sudden occlusion of the main artery of a part, whether by the impaction of an embolus or the formation of a thrombus in its lumen, when the collateral circulation is not sufficiently free to maintain the vitality of the tissues.
There is sudden pain at the site of impaction of the embolus, and the pulses beyond are lost. The limb becomes cold, numb, insensitive, and powerless. It is often pale at first—hence the term “white gangrene” sometimes applicable to the early appearances, which closely resemble those presented by the limb of a corpse.
If the part is aseptic it shrivels, and presents the ordinary features of dry gangrene. It is liable, however, especially in the lower extremity and when the veins also are obstructed, to become infected and to assume the characters of the moist type.
The extent of the gangrene depends upon the site of impaction of the embolus, thus if the abdominal aorta becomes suddenly occluded by an embolus at its bifurcation, the obstruction of the iliacs and femorals induces symmetrical gangrene of both extremities as high as the inguinal ligaments. When gangrene follows occlusion of the external iliac or of the femoral artery above the origin of its deep branch, the death of the limb extends as high as the middle or upper third of the thigh. When the femoral below the origin of its deep branch or the popliteal artery is obstructed, the veins remaining pervious, the anastomosis through the profunda is sufficient to maintain the vascular supply, and gangrene does not necessarily follow. The rupture of a popliteal aneurysm, however, by compressing the vein and the articular branches, usually determines gangrene. When an embolus becomes impacted at the bifurcation of the popliteal, if gangrene ensues it usually spreads well up the leg.
When the axillary artery is the seat of embolic impaction, and gangrene ensues, the process usually reaches the middle of the upper arm. Gangrene following the blocking of the brachial at its bifurcation usually extends as far as the junction of the lower and middle thirds of the forearm.
Gangrene due to thrombosis or embolism is sometimes met with in patients recovering from typhus, typhoid, or other fevers, such as that associated with child-bed. It occurs in peripheral parts, such as the toes, fingers, nose, or ears.
Treatment.—The general treatment of embolic gangrene is the same as that for the senile form. Success has followed opening the artery and removing the embolus. The artery is exposed at the seat of impaction and, having been clamped above and below, a longitudinal opening is made and the clot carefully extracted with the aid of forceps; it is sometimes unexpectedly long (one recorded from the femoral artery measured nearly 34 inches); the wound in the artery is then sewn up with fine silk soaked in paraffin. When amputation is indicated, it must be performed sufficiently high to ensure a free vascular supply to the flaps.
Gangrene following Ligation of Arteries.—After the ligation of an artery in its continuity—for example, in the treatment of aneurysm—the limb may for some days remain in a condition verging on gangrene, the distal parts being cold, devoid of sensation, and powerless. As the collateral circulation is established, the vitality of the tissues is gradually restored and these symptoms pass off. In some cases, however,—and especially in the lower extremity—gangrene ensues and presents the same characters as those resulting from embolism. It tends to be of the dry type. The occlusion of the vein as well as the artery is not found to increase the risk of gangrene.
Gangrene from Mechanical Constriction of the Vessels of the part.—The application of a bandage or plaster-of-Paris case too tightly, or of a tourniquet for too long a time, has been known to lead to death of the part beyond; but such cases are rare, as are also those due to the pressure of a fractured bone or of a tumour on a large artery or vein. When gangrene occurs from such causes, it tends to be of the moist type.
Much commoner is it to meet with localised areas of necrosis due to the excessive pressure of splints over bony prominences, such as the lateral malleolus, the medial condyle of the humerus, or femur, or over the dorsum of the foot. This is especially liable to occur when the nutrition of the skin is depressed by any interference with its nerve-supply, such as follows injuries to the spine or peripheral nerves, disease of the brain, or acute anterior poliomyelitis. When the splint is removed the skin pressed upon is found to be of a pale yellow or grey colour, and is surrounded by a ring of hyperæmia. If protected from infection, the clinical course is that of dry gangrene.
Bed-sores, which are closely allied to pressure sores, will be described at the end of this chapter.
When a localised portion of tissue, for example, a piece of skin, is so severely crushed or bruised that its blood vessels are occluded and its structure destroyed, it dies, and, if not infected with bacteria, dries up, and the shrivelled brown skin is slowly separated by the growth of granulation tissue beneath and around it.
Fingers, toes, or even considerable portions of limbs may in the same way be suddenly destroyed by severe trauma, and undergo mummification. If organisms gain access, typical moist gangrene may ensue, or changes similar to those of ordinary post-mortem decomposition may take place.
Treatment.—The first indication is to exclude bacteria by purifying the damaged part and its surroundings, and applying dry, non-irritating dressings.
When these measures are successful, dry gangrene ensues. The raw surface left after the separation of the dead skin may be allowed to heal by granulation, or may be covered by skin-grafts. In the case of a finger or a limb it is not necessary to wait until spontaneous separation takes place, as this is often a slow process. When a well-marked line of demarcation has formed, amputation may be performed just sufficiently far above it to enable suitable flaps to be made.
The end of a stump, after spontaneous separation of the gangrenous portion, requires to be trimmed, sufficient bone being removed to permit of the soft parts coming together.
If moist gangrene supervenes, amputation must be performed without delay, and at a higher level.
Gangrene from Heat, Chemical Agents, and Cold.—Severe burns and scalds may be followed by necrosis of tissue. So long as the parts are kept absolutely dry—as, for example, by the picric acid method of treatment—the grossly damaged portions of tissue undergo dry gangrene; but when wet or oily dressings are applied and organisms gain access, moist gangrene follows.
Strong chemical agents, such as caustic potash, nitric or sulphuric acid, may also induce local tissue necrosis, the general appearances of the lesions produced being like those of severe burns. The resulting sloughs are slow to separate, and leave deep punched-out cavities which are long of healing.
Carbolic Gangrene.—Carbolic acid, even in comparatively weak solution, is liable to induce dry gangrene when applied as a fomentation to a finger, especially in women and children. Thrombosis occurs in the blood vessels of the part, which at first is pale and soft, but later becomes dark and leathery. On account of the anæsthetic action of carbolic acid, the onset of the process is painless, and the patient does not realise his danger. A line of demarcation soon forms, but the dead part separates very slowly.
Gangrene from Frost-bite.—It is difficult to draw the line between the third degree of chilblain and the milder forms of true frost-bite; the difference is merely one of degree. Frost-bite affects chiefly the toes and fingers—especially the great toe and the little finger—the ears, and the nose. In this country it is seldom seen except in members of the tramp class, who, in addition to being exposed to cold by sleeping in the open air, are ill-fed and generally debilitated. The condition usually manifests itself after the parts, having been subjected to extreme cold, are brought into warm surroundings. The first symptom is numbness in the part, followed by a sense of weight, tingling, and finally by complete loss of sensation. The part attacked becomes white and bleached-looking, feels icy cold, and is insensitive to touch. Either immediately, or, it may be, not for several days, it becomes discoloured and swollen, and finally contracts and shrivels. Above the dead area the limb may be the seat of excruciating pain. The dead portion is cast off, as in other forms of dry gangrene, by the formation of a line of demarcation.
To prevent the occurrence of gangrene from frost-bite it is necessary to avoid the sudden application of heat. The patient should be placed in a cold room, and the part rubbed with snow, or put in a cold bath, and have light friction applied to it. As the circulation is restored the general surroundings and the local applications are gradually made warmer. Elevation of the part, wrapping it in cotton wool, and removal to a warmer room, are then permissible, and stimulants and warm drinks may be given with caution. When by these means the occurrence of gangrene is averted, recovery ensues, its onset being indicated by the white parts assuming a livid red hue and becoming the seat of an acute burning sensation.
A condition known as Trench feet was widely prevalent amongst the troops in France during the European War. Although allied to frost-bite, cold appears to play a less important part in its causation than humidity and constriction of the limbs producing ischæmia of the feet. Changes were found in the endothelium of the blood vessels, the axis cylinders of nerves, and the muscles. The condition does not occur in civil life.
Diabetic Gangrene.—This form of gangrene is prone to occur in persons over fifty years of age who suffer from glycosuria. The arteries are often markedly diseased. In some cases the existence of the glycosuria is unsuspected before the onset of the gangrene, and it is only on examining the urine that the cause of the condition is discovered. The gangrenous process seldom begins as suddenly as that associated with embolism, and, like senile gangrene, which it may closely simulate in its early stages, it not infrequently begins after a slight injury to one of the toes. It but rarely, however, assumes the dry, shrivelling type, as a rule being attended with swelling, œdema, and dusky redness of the foot, and severe pain. According to Paget, the dead part remains warm longer than in other forms of senile gangrene; there is a greater tendency for patches of skin at some distance from the primary seat of disease to become gangrenous, and for the death of tissue to extend upwards in the subcutaneous planes, leaving the overlying skin unaffected. The low vitality of the tissues favours the growth of bacteria, and if these gain access, the gangrene assumes the characters of the moist type and spreads rapidly.
The rules for amputation are the same as those governing the treatment of senile gangrene, the level at which the limb is removed depending upon whether the gangrene is of the dry or moist type. The general treatment for diabetes must, of course, be employed whether amputation is performed or not. Paget recommended that the dietetic treatment should not be so rigid as in uncomplicated diabetes, and that opium should be given freely.
The prognosis even after amputation is unfavourable. In many cases the patient dies with symptoms of diabetic coma within a few days of the operation; or, if he survives this, he may eventually succumb to diabetes. In others there is sloughing of the flaps and death results from toxæmia. Occasionally the other limb becomes gangrenous. On the other hand, the glycosuria may diminish or may even disappear after amputation.
Gangrene associated with Spasm of Blood Vessels.—Raynaud's Disease, or symmetrical gangrene, is supposed to be due to spasm of the arterioles, resulting from peripheral neuritis. It occurs oftenest in women, between the ages of eighteen and thirty, who are the subjects of uterine disorders, anæmia, or chlorosis. Cold is an aggravating factor, as the disease is commonest during the winter months. The digits of both hands or the toes of both feet are simultaneously attacked, and the disease seldom spreads beyond the phalanges or deeper than the skin.
The first evidence is that the fingers become cold, white, and insensitive to touch and pain. These attacks of local syncope recur at varying intervals for months or even years. They last for a few minutes or even for some hours, and as they pass off the parts become hyperæmic and painful.
A more advanced stage of the disease is known as local asphyxia. The circulation through the fingers becomes exceedingly sluggish, and the parts assume a dull, livid hue. There is swelling and burning or shooting pain. This may pass off in a few days, or may increase in severity, with the formation of bullæ, and end in dry gangrene. As a rule, the slough which forms is comparatively small and superficial, but it may take some months to separate. The condition tends to recur in successive winters.
The treatment consists in remedying any nervous or uterine disorder that may be present, keeping the parts warm by wrapping them in cotton wool, and in the use of hot-air or electric baths, the parts being immersed in water through which a constant current is passed. When gangrene occurs, it is treated on the same lines as other forms of dry gangrene, but if amputation is called for it is only with a view to removing the dead part.
Angio-sclerotic Gangrene.—A form of gangrene due to angio-sclerosis is occasionally met with in young persons, even in children. It bears certain analogies to Raynaud's disease in that spasm of the vessels plays a part in determining the local death.
The main arteries are narrowed by hyperplastic endarteritis followed by thrombosis, and similar changes are found in the veins. The condition is usually met with in the feet, but the upper extremity may be affected, and is attended with very severe pain, rendering sleep impossible.
The patient is liable to sudden attacks of numbness, tingling and weakness of the limbs which pass off with rest—intermittent claudication. During these attacks the large arteries—femoral, brachial, and subclavian—can be felt as firm cords, while pulsation is lost in the peripheral vessels. Gangrene eventually ensues, is attended with great pain and runs a slow course. It is treated on the same lines as Raynaud's disease.
Gangrene from Ergot.—Gangrene may occur from interference with blood supply, the result of tetanic contraction of the minute vessels, such as results in ill-nourished persons who eat large quantities of coarse rye bread contaminated with the claviceps purpurea and containing the ergot of rye. It has also occurred in the fingers of patients who have taken ergot medicinally over long periods. The gangrene, which attacks the toes, fingers, ears, or nose, is preceded by formication, numbness, and pains in the parts to be affected, and is of the dry variety.
In this country it is usually met with in sailors off foreign ships, whose dietary largely consists of rye bread. Trivial injuries may be the starting-point, the anæsthesia produced by the ergotin preventing the patient taking notice of them. Alcoholism is a potent predisposing cause.
As it is impossible to predict how far the process will spread, it is advisable to wait for the formation of a line of demarcation before operating, and then to amputate immediately above the dead part.